A widely used tool in critical care areas, point-of-care ultrasound (POCUS), allows healthcare providers to obtain the accurate diagnosis required for their patients. This can enhance the decision-making process, and it can ensure that patients can be quickly and safely evaluated. It’s for this reason that point-of-care ultrasound is gaining widespread interest and is becoming more popular. Patients can benefit from more efficient chest compression’s while being evaluated with point-of-care ultrasound, making the response to a cardiac emergency more effective than ever.
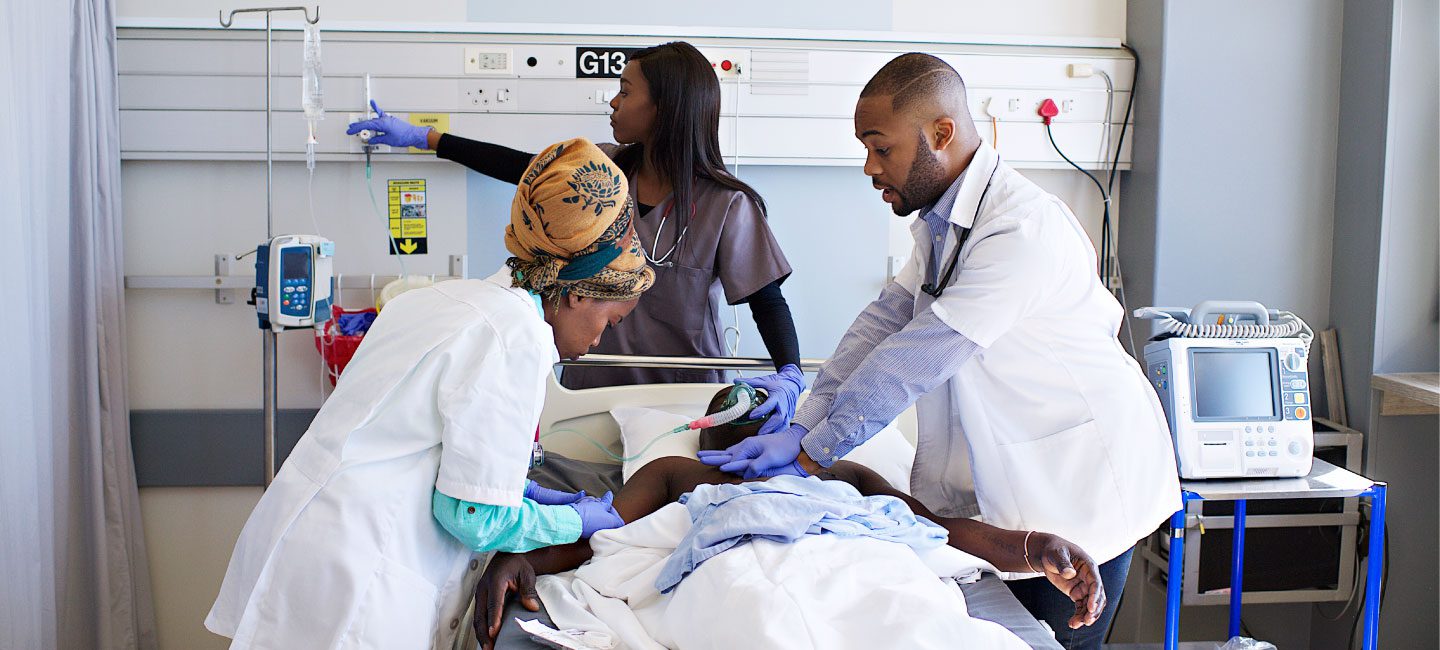
POCUS during cardiac resuscitation is controversial, but here are some of the ways it is currently used:
- The current CPR guidelines recommend performing POCUS when a reversible cause of CA is suspected. During cardiac arrest, point-of-care ultrasound has become standard to be able to reverse pericardial tamponade or to better manage cardiac standstill. It’s hard to get the right view of the heart during chest compressions, so a point-of-care ultrasound cardiac view is used in the pauses for pulse and during any rhythm checks. Too much POCUS during resuscitation and CPR can be detrimental if the pause is too long, so it becomes a balancing act.
- Monitor the overall CPR process. A patient in cardiac difficulties will benefit from CPR. This is particularly true after a sudden cardiac arrest. With the right delivery of POCUS during the CPR process, patients benefit from better outcomes and prognosis.
- Interpreting the efficacy of chest compression’s. During CPR, a physician has to apply chest compression’s between five to six centimeters 2.0 -2.5 inches. If chest compression’s aren’t effective then the oxygen supply to the brain and heart will be hampered. A rate of 100-120 compression’s per minute is essential, for better survival rates. The compression’s create blood flow to the heart and brain, which helps the oxygen to reach the heart and brain and helps to delay tissue death and provide a longer time period to do effective resuscitation of the patient in cardiac arrest.
- Distinguishing a true asystolia from a false asystolia. Patients who present as asystole often have a 0-2% survival rate, with a very poor prognosis with it. 98% of asystole patients do not survive to hospital discharge, but if their heart rhythm is shockable early enough, the prognosis is slightly better. It’s essential to know that not all asystole is true asystole, as false asystole can appear on a bedside monitor due to a technical error.There is more than one way to measure asystole, including recording patient conditions, movement artifact, and point-of-care ultrasound. It’s considered to be dangerous to deliver shocks during a cardiac arrest during asystole, as it can lead to a parasympathetic storm. When it comes to asystole, the right approach is crucial to success and patient survival rates. To determine the difference between real and false asystole, POCUS is needed to view the heart. True asystole should never be shocked in a cardiac arrest, but once false asystole is established, a shock can help, and clinicians can use point-of-care ultrasound to determine this.
- Diagnosis of reversible causes of cardiac arrest, such as tamponade, tension pneumothorax and hypovolemia. Treating the causes of cardiac arrest is the most crucial component in the improvement of patient outcomes. Most of the cases of cardiac arrest are reversible, and this includes the conditions below:Hypoxia: It’s not common for cardiac arrest to be caused by pure hypoxemia. This is when low levels of oxygen are circulating the blood. Over time, this leads to hypoxia at the tissues. This is usually a direct consequence of asphyxia, and this is one of the most common causes of cardiac arrest. You must treat hypoxia symptoms quickly. Given that this is one of the most common causes of reversible cardiac arrest, the proper oxygenation is key to negating an abnormal cardiac rhythm. Other common causes of cardiac arrest include:
- Airway obstruction: soft tissues (coma), laryngospasm, aspiration
- Anemia
- Asthma
- Chronic obstructive pulmonary disease
- Drowning
- Hanging
- High altitude
- Impaired alveolar ventilation from neuromuscular disease
- Pneumonia
- Tension pneumothorax
- Trauma
POCUS used to be a rarity in clinical care. Still, it’s increasingly the first port of call for clinicians looking for a fast diagnosis and to provide better patient care. Higher patient satisfaction leads to better outcomes for the facility using POCUS as standard practice.
Looking for additional inspiration? Sign up for our POCUS Post™ newsletter to receive monthly tips and ideas.





















