Victor V Rao MBBS, DMRD, RDMS- Abdomen, Ob/Gyn (APCA)
Introduction
Molar pregnancy is the most common type of gestational trophoblastic disease (GTD). It is also known as a hydatidiform mole. It is a commonly encountered condition with an incidence of approximately 1 in every 1000-2000 pregnancies. If you regularly perform first and second-trimester point-of-care ultrasound (POCUS) examinations on pregnant patients, you will come across some patients with this condition. All clinicians performing first, and second-trimester ultrasound examinations must be aware of this condition and its sonographic findings. Women in their teens and the forty to fifty age groups appear to have a higher incidence. A molar pregnancy is rarely seen with a documented normal intrauterine pregnancy (IUP).
Types of Molar Pregnancies
There are two types of molar pregnancies.
- Partial molar pregnancy
- Complete molar pregnancy
In partial moles, the karyotype is usually triploid (69, XXY). It is the result of fertilization of a normal egg by two sperm, one bearing a 23, X chromosomal pattern and the other a 23Y chromosomal pattern. Only 0.1% of partial molar pregnancies have a risk of persistent trophoblastic disease or malignancy. The serum beta-HCG levels may still be within the wide range of a normal intrauterine pregnancy.
Complete molar pregnancy has 46, XX diploid chromosomal pattern and infrequently has 46, XY karyotype. All the chromosomes are derived from a single sperm in 90% of cases or less commonly two sperms, suggesting fertilization of a single egg that has lost its chromosomes.
Molar pregnancies are commonly seen implanted within the uterine cavity and very seldom in an ectopic location such as the fallopian tube or ovary. Complete molar pregnancies have a much higher risk of persistent trophoblastic disease or choriocarcinoma. The serum beta-HCG levels are markedly elevated in a complete molar pregnancy and may exceed 100,000 IU/L.
Clinical Presentation
Molar pregnancy may be suspected in patients who present with the following:
- Abnormal vaginal bleeding in early pregnancy
- Pelvic pain
- Hyperemesis
- Vaginal passage of grape-like vesicles
- Uterus large for date
Ultrasound Findings of a Complete Molar Pregnancy
In a complete molar pregnancy, the following ultrasound findings may be visible:
- Enlarged or bulky uterus
- Mass with cystic structures
- Snowstorm or bunch of grapes appearance
- < 50% may be diagnosed in the first trimester
- It may appear like a normal IUP
- It may appear like an empty gestational sac
- Large cysts may be seen in the ovaries—theca lutein cysts
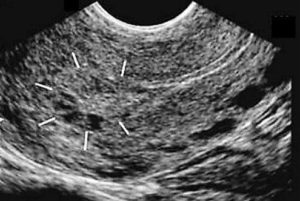
Figure 1. Complete molar pregnancy. Image courtesy- Fetalultrasound.com
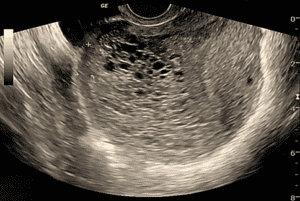
Figure 2. Complete molar pregnancy. Observe the enlarged uterus with some cystic anechoic lesions and snowstorm appearance in the rest of the uterine cavity. No definite fetus or fetal parts are seen.

Figure 3. Picture taken during a snowstorm
Ultrasound Findings of a Partial Molar Pregnancy
The following ultrasound findings may be seen in a partial molar pregnancy:
- Fetus or fetal parts seen
- Developmental anomalies of the fetus seen
- Evidence of growth restriction of the fetus
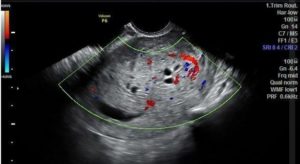
Figure 4. Enlarged uterus with a small irregular gestational sac. A non-viable embryo was seen. The placenta is thick and hyperechoic with multiple small anechoic spaces and increased blood flow on color Doppler. Findings are consistent with partial molar pregnancy. Image courtesy Radiopedia.org. See reference.
Differential Diagnosis
- *Uterine sarcoma
- *Uterine lymphangioma
- *Uterine dysgerminoma
* Unlike complete molar pregnancy, the b-HCG and a-fetoprotein levels are not elevated in these conditions.
Conclusion
Molar pregnancy must be diagnosed and treated effectively. Follow-ups are required to assess for serious complications due to persistent gestational trophoblastic disease. Partial molar pregnancy is at a much lower risk for complications as compared to a complete molar pregnancy.
Reference
Anan, R.A. (n.d.). Partial molar pregnancy. Radiopaedia. Retrieved December 2022. https://radiopaedia.org/cases/partial-molar-pregnancy-2?lang=us
Access the full POCUS Learning Library for FREE!
Share a few details so we can tailor new content to your specialty and region.




















